Key takeaways:
~ GLP-1, a hormone released in the intestines and brain, regulates appetite and blood sugar by signaling insulin release and suppressing glucagon.
~ Acute stress and large meals trigger GLP-1 in the brain to suppress appetite, preventing overeating.
~ GLP-1 receptor agonists and natural inhibitors of its degradation may help with weight loss.
~ Genetic variants in GLP1 genes are linked to obesity and diabetes.
Glucagon-like Peptide-1(GLP-1) signals that you’ve just eaten
Food reaching your intestines for absorption triggers the release of certain hormones. These signals can tell your brain that you’re no longer hungry and tell the pancreas to release insulin.
One of these hormones is called GLP-1, a glucagon-like peptide-1.
GLP-1 is a peptide hormone (a small protein molecule) that is released in the upper part of the intestinal tract when you eat carbohydrates or certain proteins. It is classified as an incretin, which helps regulate blood glucose levels.
The GLP-1 peptide hormone signals the body when food consumption occurs. The GLP-1 receptor (GLP1R), found in pancreatic beta cells, receives the signal triggering the release of insulin. It also targets other cells in the pancreas to stop the glucagon signal for generating glucose in the liver.[ref]
Additionally, GLP-1 is created in the brain and acts as a neuropeptide. More on this in a minute…
Let’s back up a sec and talk about proglucagon…
Proglucagon is a big molecule that can be chopped apart to form other molecules — including GLP-1. Preproglucagon is encoded by the GCG gene and cleaved into proglucagon.
Both the pancreas (alpha cells) and the intestines can make proglucagon.
Controlling glucose levels: In the pancreas, the proglucagon can convert into glucagon, which in turn signals the liver to release glucose. The alpha cells in the pancreas secrete proglucagon when blood glucose levels are low. The release of proglucagon causes the liver to make glucose (gluconeogenesis – converting protein to glucose) as well as to convert fatty acids into ketone bodies.
Intestinal proglucagon cleaves (breaks up) into several different molecules:
- GLP-1
- GLP-2
- GRPP
- Oxyntomodulin
The enzyme PCSK1 converts proglucagon to GLP-1 in the central nervous system. (We’ll come back to this in the genetics section)
Here’s a diagram of the possible cleaving of proglucagon:
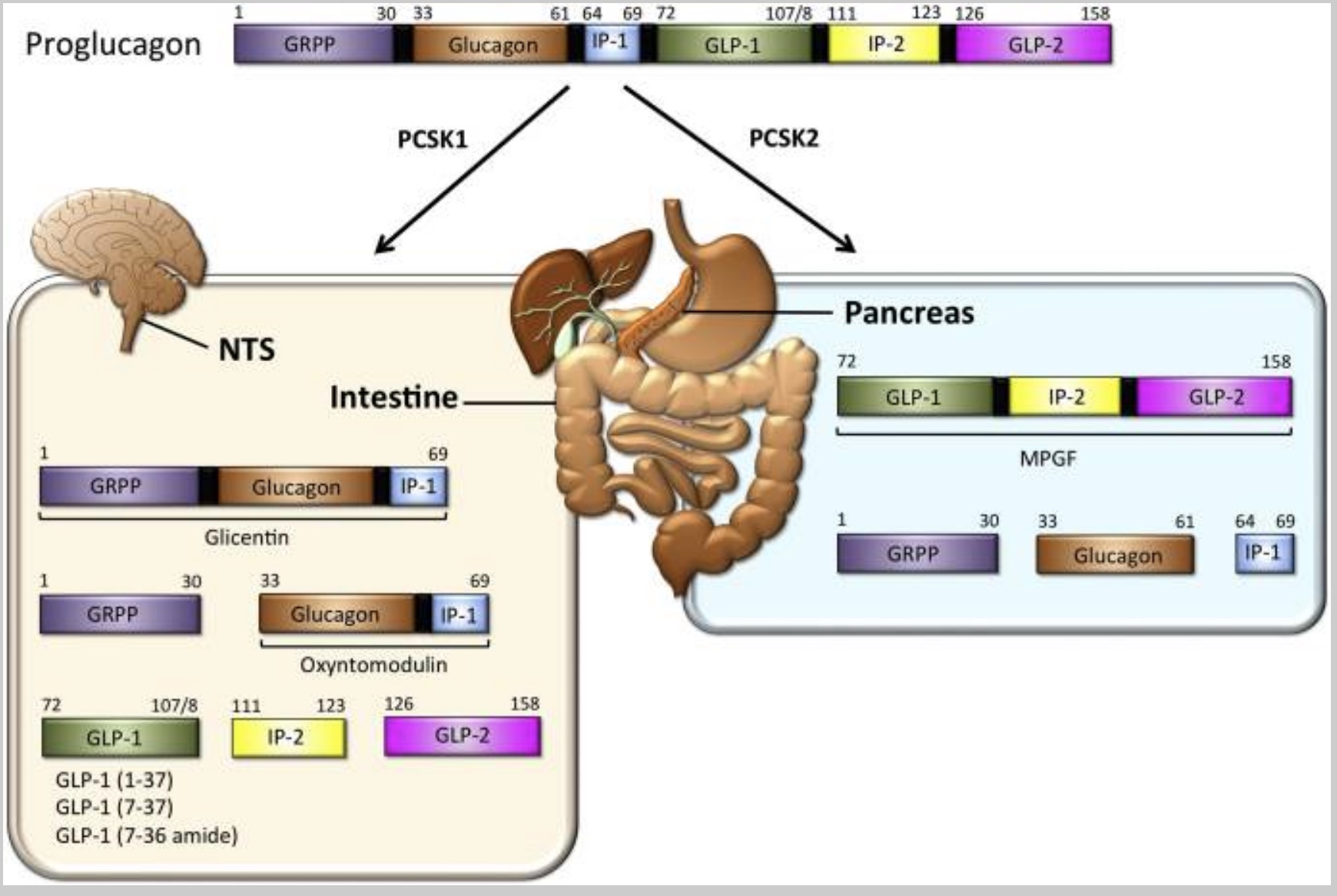
GLP-1 signal to the pancreas:
The GLP-1 hormone doesn’t stick around long. With a half-life of around 2 minutes, this quick signal is rapidly degraded by the protein DPP-4 (dipeptidyl peptidase 4).
Thus, only about 10-15% of released GLP-1 reaches the pancreas as a signal.
The GLP-1 that does reach the pancreas calls for the release of more insulin when food is being broken down and absorbed. Plus, it stops the production of glucagon, thus decreasing glucose from the liver.
The effects of GLP-1 are completed through its binding to the GLP-1 receptor (GLP1R).
Are GLP-1 levels genetic?
The heritability of GLP-1 release is around 50%.[ref] Thus, while there is a fairly important genetic component, diet is also really important.
Common genetic variants in the GLP1R (GLP-1 receptor) gene impact weight and type 2 diabetes risk.
GLP-1 and appetite suppression:
I mentioned above that the intestines and the brain make GLP-1.
Certain areas of the hypothalamus can make GLP-1, as well as regions of the brain stem. Plus, GLP-1 is involved in stress response and the HPA axis.[ref]
Different regions in the brain control your desire to eat, and GLP-1 comes into play here in specific ways.
Specific neurons in the brain stem control swallowing, intestinal movements — and stress-induced loss of appetite. (The brain stem also controls other involuntary functions such as heartbeat and breathing.)
GLP-1 in the brain stem activates due to stress and causes a loss of appetite. Researchers have figured this out by using transgenic mice in which they can turn off the GLP-1 in the brain to see what happens. The researchers found that turning off GLP-1 in the brain didn’t affect the normal daily intake of food, but instead was important in several specific situations: prolonged fasting, large feedings, and stress-induced appetite loss.[ref]
Essentially, the neurons activated by GLP-1 help to limit binging after a fast – they keep you from massively overeating after not eating for a while.
The GLP-1-activated neurons in the brain also limit appetite for a while after a large meal (e.g., the thought of eating is unappealing for many hours after pigging out on pizza).[ref]
Additionally, the GLP-1 neurons activate during times of acute stress to suppress appetite. We all have experienced that loss of appetite during stressful situations – when the thought of eating food just doesn’t cross the mind.
The GLP-1 produced in the intestines after a meal also plays a role in suppressing eating, likely through different circuits than those GLP-1-expressing neurons found in the brain stem. Researchers think that this involves the vagus nerve.[ref]
GLP-1 receptor agonist drugs:
Recent clinical trials show that drugs that activate GLP-1 receptors, such as liraglutide or semaglutide (diabetes drugs), cause gradual weight loss in obese people. This may be due to decreasing the amount eaten after fasting – limiting a binge – or increasing the appetite suppression longer after eating a big meal.
The drawback to these drugs is that they are administered as weekly injections, and it isn’t known if the weight loss is permanent.
GLP-1 and immune response:
In addition to their role in pancreatic insulin secretion, GLP-1 receptors are found in certain types of immune cells, including T cells and macrophages.[ref] This is an interesting link between metabolic health and immune health.
The receptor for GLP-1 is found on the cell membrane of macrophages, regulatory T cells, and natural killer T cells. GLP-1 plays an immunomodulatory role. A GLP-1 receptor agonist medication may help patients with psoriasis.[ref]
Asthma exacerbations also decreased in patients on GLP-1 receptor agonist medications.[ref]
GLP-1 and Alzheimer’s disease:
In animal studies, infusions of GLP-1 decrease amyloid-beta levels and prevent neuronal cell death.[ref]
Dysregulation of glucose entry into the brain is one hallmark of Alzheimer’s disease, tying together insulin resistance, GLP-1, and dementia.[ref][ref] GLP-1 receptor agonist drugs, such as liraglutide, are being studied for Alzheimer’s disease.[ref]
Role of Circadian Rhythm in GLP-1:
Circadian rhythm is the 24-hour rhythm of your body’s functions. It controls when hormones are released, the production of enzymes at different times of the day, immune response during the day vs. night, sleep-wake timing, and much more.
Like many hormones, there is a circadian aspect to GLP-1. Research points to GLP-1 as having a role in entraining the circadian rhythm of insulin release in the pancreas. While GLP-1 will be released from intestinal cells upon consumption of food, the amount of insulin release caused by GLP-1 varies due to the time of day.[ref]
A ‘Western Diet’, high in fat and sugar, is used in research studies to make animals fat. This type of diet actually alters the rhythm of GLP-1 secretion in animal studies and in people with type 2 diabetes.[ref]
What is the role of DPP-4?
Again, the half-life of GLP-1 is really short – about 2 minutes – because a ubiquitous protein-degrading enzyme called DPP-4 breaks it down quickly.
Blocking the degradation of GLP-1 by inhibiting DPP-4 is one way certain types of diabetes medicine work.
GLP-1 Genotype Report
Lifehacks:
Increasing GLP1 through binding to the GLP-1 receptor has been shown to slowly reduce weight in people who are obese.[ref]
Supplements that increase GLP-1:
Keep in mind that GLP-1 is quickly broken down in the body. The effects of supplements that increase GLP-1 may not last long. Theoretically, increasing GLP-1 before a meal may decrease appetite and the amount eaten.
Natural DPP4 inhibitors:
Related Articles and Topics:
Intermittent Fasting: Benefits from changing Gene Expression
References:
Brierley, Daniel I., et al. “Central and Peripheral GLP-1 Systems Independently Suppress Eating.” Nature Metabolism, vol. 3, no. 2, Feb. 2021, pp. 258–73. PubMed Central, https://doi.org/10.1038/s42255-021-00344-4.
—. “Central and Peripheral GLP-1 Systems Independently Suppress Eating.” Nature Metabolism, vol. 3, no. 2, Feb. 2021, pp. 258–73. PubMed Central, https://doi.org/10.1038/s42255-021-00344-4.
Chedid, V., et al. “Allelic Variant in the Glucagon-like Peptide 1 Receptor Gene Associated with Greater Effect of Liraglutide and Exenatide on Gastric Emptying: A Pilot Pharmacogenetics Study.” Neurogastroenterology and Motility: The Official Journal of the European Gastrointestinal Motility Society, vol. 30, no. 7, July 2018, p. e13313. PubMed, https://doi.org/10.1111/nmo.13313.
de Graaf, Chris, et al. “Glucagon-Like Peptide-1 and Its Class B G Protein–Coupled Receptors: A Long March to Therapeutic Successes.” Pharmacological Reviews, vol. 68, no. 4, Oct. 2016, pp. 954–1013. PubMed Central, https://doi.org/10.1124/pr.115.011395.
—. “Glucagon-Like Peptide-1 and Its Class B G Protein–Coupled Receptors: A Long March to Therapeutic Successes.” Pharmacological Reviews, vol. 68, no. 4, Oct. 2016, pp. 954–1013. PubMed Central, https://doi.org/10.1124/pr.115.011395.
Diz-Chaves, Yolanda, et al. “Glucagon-Like Peptide-1 (GLP-1) in the Integration of Neural and Endocrine Responses to Stress.” Nutrients, vol. 12, no. 11, Oct. 2020, p. 3304. PubMed Central, https://doi.org/10.3390/nu12113304.
Eser, Hale Yapici, et al. “Association Between GLP-1 Receptor Gene Polymorphisms with Reward Learning, Anhedonia, and Depression Diagnosis.” Acta Neuropsychiatrica, vol. 32, no. 4, Aug. 2020, pp. 218–25. PubMed Central, https://doi.org/10.1017/neu.2020.14.
Femminella, Grazia Daniela, et al. “Evaluating the Effects of the Novel GLP-1 Analogue Liraglutide in Alzheimer’s Disease: Study Protocol for a Randomised Controlled Trial (ELAD Study).” Trials, vol. 20, no. 1, Apr. 2019, p. 191. PubMed, https://doi.org/10.1186/s13063-019-3259-x.
Foer, Dinah, et al. “Asthma Exacerbations in Patients with Type 2 Diabetes and Asthma on Glucagon-like Peptide-1 Receptor Agonists.” American Journal of Respiratory and Critical Care Medicine, vol. 203, no. 7, Apr. 2021, pp. 831–40. PubMed, https://doi.org/10.1164/rccm.202004-0993OC.
Gejl, Michael, et al. “Blood-Brain Glucose Transfer in Alzheimer’s Disease: Effect of GLP-1 Analog Treatment.” Scientific Reports, vol. 7, no. 1, Dec. 2017, p. 17490. PubMed, https://doi.org/10.1038/s41598-017-17718-y.
Geraedts, Maartje C. P., et al. “Direct Induction of CCK and GLP-1 Release from Murine Endocrine Cells by Intact Dietary Proteins.” Molecular Nutrition & Food Research, vol. 55, no. 3, Mar. 2011, pp. 476–84. PubMed, https://doi.org/10.1002/mnfr.201000142.
“Glutamine: Benefits, Uses and Side Effects.” Healthline, 13 Jan. 2018, https://www.healthline.com/nutrition/glutamine.
Greenfield, Jerry R., et al. “Oral Glutamine Increases Circulating GLP-1, Glucagon and Insulin Levels in Lean, Obese and Type 2 Diabetic Subjects.” The American Journal of Clinical Nutrition, vol. 89, no. 1, Jan. 2009, pp. 106–13. PubMed Central, https://doi.org/10.3945/ajcn.2008.26362.
Heo, Chan Uk, and Chang-Ik Choi. “Current Progress in Pharmacogenetics of Second-Line Antidiabetic Medications: Towards Precision Medicine for Type 2 Diabetes.” Journal of Clinical Medicine, vol. 8, no. 3, Mar. 2019, p. 393. PubMed Central, https://doi.org/10.3390/jcm8030393.
—. “Current Progress in Pharmacogenetics of Second-Line Antidiabetic Medications: Towards Precision Medicine for Type 2 Diabetes.” Journal of Clinical Medicine, vol. 8, no. 3, Mar. 2019, p. 393. PubMed Central, https://doi.org/10.3390/jcm8030393.
Hira, Tohru, et al. “Improvement of Glucose Tolerance by Food Factors Having Glucagon-Like Peptide-1 Releasing Activity.” International Journal of Molecular Sciences, vol. 22, no. 12, June 2021, p. 6623. PubMed Central, https://doi.org/10.3390/ijms22126623.
Hogan, A. E., et al. “Glucagon-like Peptide-1 (GLP-1) and the Regulation of Human Invariant Natural Killer T Cells: Lessons from Obesity, Diabetes and Psoriasis.” Diabetologia, vol. 54, no. 11, Nov. 2011, pp. 2745–54. PubMed, https://doi.org/10.1007/s00125-011-2232-3.
Holt, Marie K., et al. “Preproglucagon Neurons in the Nucleus of the Solitary Tract Are the Main Source of Brain GLP-1, Mediate Stress-Induced Hypophagia, and Limit Unusually Large Intakes of Food.” Diabetes, vol. 68, no. 1, Jan. 2019, pp. 21–33. PubMed Central, https://doi.org/10.2337/db18-0729.
Jarvela, Timothy S., et al. “Reduced Stability and PH-Dependent Activity of a Common Obesity-Linked PCSK1 Polymorphism, N221D.” Endocrinology, vol. 160, no. 11, Nov. 2019, pp. 2630–45. PubMed, https://doi.org/10.1210/en.2019-00418.
Jensterle, Mojca, et al. “Genetic Variability in GLP-1 Receptor Is Associated with Inter-Individual Differences in Weight Lowering Potential of Liraglutide in Obese Women with PCOS: A Pilot Study.” European Journal of Clinical Pharmacology, vol. 71, no. 7, July 2015, pp. 817–24. PubMed, https://doi.org/10.1007/s00228-015-1868-1.
—. “Genetic Variability in GLP-1 Receptor Is Associated with Inter-Individual Differences in Weight Lowering Potential of Liraglutide in Obese Women with PCOS: A Pilot Study.” European Journal of Clinical Pharmacology, vol. 71, no. 7, July 2015, pp. 817–24. PubMed, https://doi.org/10.1007/s00228-015-1868-1.
Kato, Masaki, et al. “Curcumin Improves Glucose Tolerance via Stimulation of Glucagon-like Peptide-1 Secretion.” Molecular Nutrition & Food Research, vol. 61, no. 3, Mar. 2017. PubMed, https://doi.org/10.1002/mnfr.201600471.
Kulanuwat, Sirikul, et al. “Effects of PCSK1 Genetic Variants on Obesity among Thai Children and Their Family Members: In Relation to Health Risk, and Biochemical and Anthropometric Parameters.” The Southeast Asian Journal of Tropical Medicine and Public Health, vol. 45, no. 1, Jan. 2014, pp. 214–25.
Löffler, Dennis, et al. “Functional and Clinical Relevance of Novel and Known PCSK1 Variants for Childhood Obesity and Glucose Metabolism.” Molecular Metabolism, vol. 6, no. 3, Mar. 2017, pp. 295–305. PubMed, https://doi.org/10.1016/j.molmet.2016.12.002.
Martchenko, Alexandre, and Patricia Lee Brubaker. “Effects of Obesogenic Feeding and Free Fatty Acids on Circadian Secretion of Metabolic Hormones: Implications for the Development of Type 2 Diabetes.” Cells, vol. 10, no. 9, Sept. 2021, p. 2297. www.mdpi.com, https://doi.org/10.3390/cells10092297.
—. “Effects of Obesogenic Feeding and Free Fatty Acids on Circadian Secretion of Metabolic Hormones: Implications for the Development of Type 2 Diabetes.” Cells, vol. 10, no. 9, Sept. 2021, p. 2297. www.mdpi.com, https://doi.org/10.3390/cells10092297.
Mbikay, Majambu, et al. “Effects of Rs6234/Rs6235 and Rs6232/Rs6234/Rs6235 PCSK1 Single-Nucleotide Polymorphism Clusters on Proprotein Convertase 1/3 Biosynthesis and Activity.” Molecular Genetics and Metabolism, vol. 104, no. 4, Dec. 2011, pp. 682–87. PubMed, https://doi.org/10.1016/j.ymgme.2011.09.027.
—. “Effects of Rs6234/Rs6235 and Rs6232/Rs6234/Rs6235 PCSK1 Single-Nucleotide Polymorphism Clusters on Proprotein Convertase 1/3 Biosynthesis and Activity.” Molecular Genetics and Metabolism, vol. 104, no. 4, Dec. 2011, pp. 682–87. PubMed, https://doi.org/10.1016/j.ymgme.2011.09.027.
Meek, Claire L., et al. “The Effect of Encapsulated Glutamine on Gut Peptide Secretion in Human Volunteers.” Peptides, vol. 77, Mar. 2016, pp. 38–46. PubMed, https://doi.org/10.1016/j.peptides.2015.10.008.
Müller, T. D., et al. “Glucagon-like Peptide 1 (GLP-1).” Molecular Metabolism, vol. 30, Sept. 2019, pp. 72–130. PubMed Central, https://doi.org/10.1016/j.molmet.2019.09.010.
—. “Glucagon-like Peptide 1 (GLP-1).” Molecular Metabolism, vol. 30, Sept. 2019, pp. 72–130. PubMed Central, https://doi.org/10.1016/j.molmet.2019.09.010.
Perry, TracyAnn, et al. “Glucagon-like Peptide-1 Decreases Endogenous Amyloid-Beta Peptide (Abeta) Levels and Protects Hippocampal Neurons from Death Induced by Abeta and Iron.” Journal of Neuroscience Research, vol. 72, no. 5, June 2003, pp. 603–12. PubMed, https://doi.org/10.1002/jnr.10611.
Pham, Hung, et al. “A Bitter Pill for Type 2 Diabetes? The Activation of Bitter Taste Receptor TAS2R38 Can Stimulate GLP-1 Release from Enteroendocrine L-Cells.” Biochemical and Biophysical Research Communications, vol. 475, no. 3, July 2016, pp. 295–300. PubMed Central, https://doi.org/10.1016/j.bbrc.2016.04.149.
Qi, Qibin, et al. “Association of PCSK1 Rs6234 with Obesity and Related Traits in a Chinese Han Population.” PloS One, vol. 5, no. 5, May 2010, p. e10590. PubMed, https://doi.org/10.1371/journal.pone.0010590.
Saleh, Rofida A., et al. “Peganum Harmala Enhanced GLP-1 and Restored Insulin Signaling to Alleviate AlCl3-Induced Alzheimer-like Pathology Model.” Scientific Reports, vol. 11, no. 1, June 2021, p. 12040. PubMed, https://doi.org/10.1038/s41598-021-90545-4.
Sheikh, Haroon I., et al. “Glucagon-Like Peptide-1 Receptor Gene Polymorphism (Leu260Phe) Is Associated With Morning Cortisol in Preschoolers.” Progress in Neuro-Psychopharmacology & Biological Psychiatry, vol. 34, no. 6, Aug. 2010, pp. 980–83. PubMed Central, https://doi.org/10.1016/j.pnpbp.2010.05.007.
Singla, Rajeev K., et al. “Natural Products: Potential Source of DPP-IV Inhibitors.” Current Protein & Peptide Science, vol. 20, no. 12, 2019, pp. 1218–25. PubMed, https://doi.org/10.2174/1389203720666190502154129.
Torekov, S. S., et al. “Homozygous Carriers of the G Allele of Rs4664447 of the Glucagon Gene (GCG) Are Characterised by Decreased Fasting and Stimulated Levels of Insulin, Glucagon and Glucagon-like Peptide (GLP)-1.” Diabetologia, vol. 54, no. 11, Nov. 2011, pp. 2820–31. PubMed, https://doi.org/10.1007/s00125-011-2265-7.
Vrang, Niels, et al. “Gastric Distension Induces C-Fos in Medullary GLP-1/2-Containing Neurons.” American Journal of Physiology. Regulatory, Integrative and Comparative Physiology, vol. 285, no. 2, Aug. 2003, pp. R470-478. PubMed, https://doi.org/10.1152/ajpregu.00732.2002.
Wessel, Jennifer, et al. “Low-Frequency and Rare Exome Chip Variants Associate with Fasting Glucose and Type 2 Diabetes Susceptibility.” Nature Communications, vol. 6, Jan. 2015, p. 5897. PubMed Central, https://doi.org/10.1038/ncomms6897.
Yildirim Simsir, Ilgin, et al. “Glucagon like Peptide-1 (GLP-1) Likes Alzheimer’s Disease.” Diabetes & Metabolic Syndrome, vol. 12, no. 3, May 2018, pp. 469–75. PubMed, https://doi.org/10.1016/j.dsx.2018.03.002.
—. “Glucagon like Peptide-1 (GLP-1) Likes Alzheimer’s Disease.” Diabetes & Metabolic Syndrome, vol. 12, no. 3, May 2018, pp. 469–75. PubMed, https://doi.org/10.1016/j.dsx.2018.03.002.
Yue, Xiao, et al. “Berberine Activates Bitter Taste Responses of Enteroendocrine STC-1 Cells.” Molecular and Cellular Biochemistry, vol. 447, no. 1–2, Oct. 2018, pp. 21–32. PubMed, https://doi.org/10.1007/s11010-018-3290-3.

