Key takeaways:
~ Exposure to childhood trauma, such as exposure to abuse, violence, or repeated stress, can have a long-lasting effect.
~ Adults exposed to childhood trauma have higher rates of depression, PTSD, suicide, and anxiety disorders.
~ Genetics is a big part of resilience to childhood trauma. For some, childhood trauma causes physiological changes that last a lifetime.
Background on cortisol:
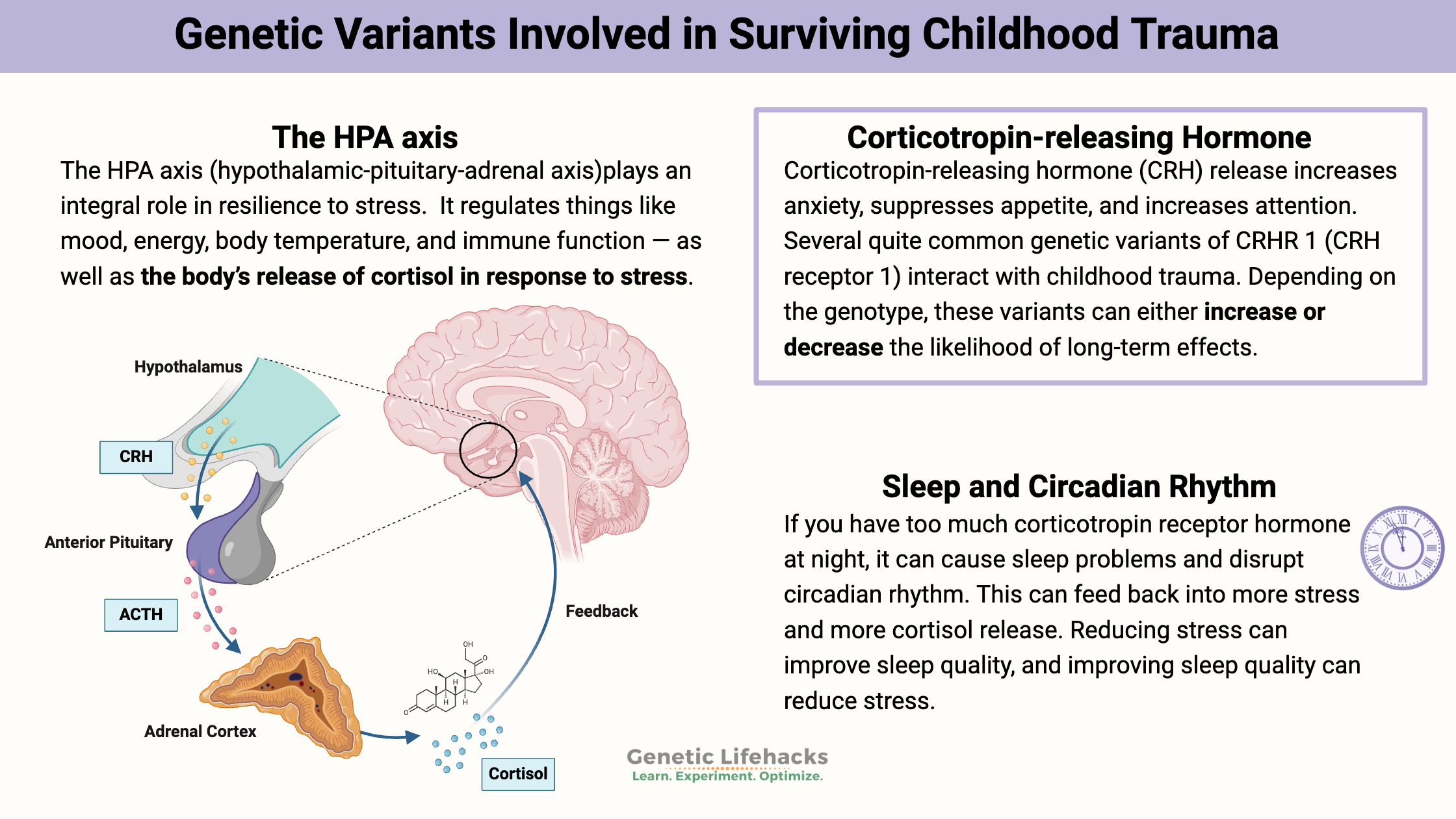
The HPA axis:
The HPA axis (hypothalamic-pituitary-adrenal axis) may play an integral role in resilience to stress. Several studies have investigated the role of the HPA axis, childhood adversity, and adult depression or anxiety.[ref] One study concluded, “A history of childhood trauma has long-standing effects on adulthood cortisol responses to stress, particularly in that depressed individuals with a history of childhood trauma show blunted cortisol responses”.[ref]
The HPA axis is basically the interactions and feedback loops between the brain (hypothalamus) and the pituitary and adrenal glands. It regulates things like mood, energy, body temperature, and immune function — as well as the body’s release of cortisol in response to stress.
Related Article: HPA Axis Dysfunction and Genetics
Corticotropin-releasing hormone:
The production of Corticotropin-releasing hormone (CRH) occurs in the hypothalamus. CRH, in turn, activates ACTH (adrenocorticotropic hormone). ACTH controls the synthesis of cortisol, mineralocorticoids, and DHEA. So it is a pathway that starts in the brain and ends with the release of hormones, such as cortisol, from the adrenal glands.
For example, CRH release increases anxiety, suppresses appetite, and increases attention – just what you need when a tiger is chasing you, but not good when it is chronically a little elevated. Cortisol levels naturally rise and fall over the course of the day in rhythm with your body’s circadian clock. There can be a cascade of chronic effects if this rhythm is either out of phase or dampened.
CRH also activates the corticotropin-releasing hormone receptor CRHR1. Several quite common genetic variants of CRHR 1 seem to interact with childhood trauma. Depending on the genotype, these variants can either increase or decrease the likelihood of long-term effects.
These genetic differences might indicate why some adults have lasting problems with cortisol (or ‘adrenal fatigue’) if exposed to traumatic events in childhood – or had chronic stress in their childhood. Or, to put it the opposite way, these variants are why some adults have no long-term problems from childhood trauma.
Resilience Genotype Report:
Lifehacks:
Talk to your doctor:
If you carry the risk variants and deal with depression or anxiety, talk with your doctor about getting your cortisol levels tested to see if your levels are lower than normal or chronically high. Ask about testing at multiple times during the day to see how your cortisol level rises and falls.
Related Articles and Topics:
Cortisol and HPA Axis Dysfunction
Cortisol is a hormone produced by the adrenal glands in times of stress, and it also plays many roles in your normal bodily functions. It is a multi-purpose hormone that needs to be in the right amount (not too high, not too low) and at the right time. Your genes play a big role in how likely you are to have problems with cortisol.
Is inflammation causing your depression or anxiety?
Research over the past two decades clearly shows a causal link between increased inflammatory markers and depression. Genetic variants in the inflammatory-related genes can increase the risk of depression and anxiety.
Lithium Orotate + B12: Boosting mood and decreasing anxiety, for some people…
For some people, low-dose, supplemental lithium orotate is a game-changer for mood issues when combined with vitamin B12. But other people may have little to no response. The difference may be in your genes.
References:
Gannon, Robert L., and Mark J. Millan. “The Corticotropin-Releasing Factor (CRF)(1) Receptor Antagonists CP154,526 and DMP695 Inhibit Light-Induced Phase Advances of Hamster Circadian Activity Rhythms.” Brain Research, vol. 1083, no. 1, Apr. 2006, pp. 96–102. PubMed, https://doi.org/10.1016/j.brainres.2006.02.017.
Gillespie, Charles F., et al. “Risk and Resilience: Genetic and Environmental Influences on Development of the Stress Response.” Depression and Anxiety, vol. 26, no. 11, 2009, pp. 984–92. PubMed Central, https://doi.org/10.1002/da.20605.
Heim, Christine, et al. “The Link between Childhood Trauma and Depression: Insights from HPA Axis Studies in Humans.” Psychoneuroendocrinology, vol. 33, no. 6, July 2008, pp. 693–710. PubMed, https://doi.org/10.1016/j.psyneuen.2008.03.008.
Jothie Richard, Edwin, et al. “Anti-Stress Activity of Ocimum Sanctum: Possible Effects on Hypothalamic-Pituitary-Adrenal Axis.” Phytotherapy Research: PTR, vol. 30, no. 5, May 2016, pp. 805–14. PubMed, https://doi.org/10.1002/ptr.5584.
Panossian, Alexander, et al. “Novel Molecular Mechanisms for the Adaptogenic Effects of Herbal Extracts on Isolated Brain Cells Using Systems Biology.” Phytomedicine, vol. 50, Nov. 2018, pp. 257–84. ScienceDirect, https://doi.org/10.1016/j.phymed.2018.09.204.
Suzuki, Akiko, et al. “Long Term Effects of Childhood Trauma on Cortisol Stress Reactivity in Adulthood and Relationship to the Occurrence of Depression.” Psychoneuroendocrinology, vol. 50, Dec. 2014, pp. 289–99. PubMed, https://doi.org/10.1016/j.psyneuen.2014.09.007.
Tyrka, Audrey R., et al. “Interaction of Childhood Maltreatment with the Corticotropin-Releasing Hormone Receptor Gene: Effects on HPA Axis Reactivity.” Biological Psychiatry, vol. 66, no. 7, Oct. 2009, pp. 681–85. PubMed Central, https://doi.org/10.1016/j.biopsych.2009.05.012.